As a leader in the aging and disability networks, you can often see where you need to take your organization to be better prepared to work with health care partners and other new payers. But getting folks on board with your vision may be challenging. We all resist change for any number of reasons, including:
- When we don’t see a clear reason for it
- When we are daunted by the amount we’ll have to learn/relearn to achieve it
- When we simply (and often incorrectly) believe it doesn’t “fit us”
Leading your organization through a transformation of culture means embracing and accepting these three core reasons on a very basic and human level, and meeting your staff and Board members where they are in their readiness to embrace change. Creating the vision is necessary and important, but the hard work of changing minds begins with a message that your staff and board of directors can truly understand.
Let’s take this apart and identify why some within your organization may simply not see “the clear reason for change,” and explore solutions to overcome resistance.
Begin by helping skeptics visualize a future for your organization where its vibrancy and strength are enhanced by its integration with key health care players; where the nature of health care delivery has changed and now embraces all the social determinants of health; and where your consumers are living longer, more independent lives, benefiting from a higher quality of care that is both affordable and accessible. This is a future worth working towards. And it is one that can galvanize your staff and other stakeholders into coming together to achieve success.
As leaders, we are often frustrated on behalf of our consumers, concerned that the care they receive is fragmented, and driven by financial incentives that are not aligned with quality and person-centeredness. And we all fear that the current health care delivery system will continue to squeeze consumers’ wallets, making basic health care unaffordable for millions. Our role as leaders of aging and disability organizations in partnering with health care will raise awareness of how the health care sector can be more sensitive to the challenges our consumers face each and every day. We need to recognize that without our self-advocating, health care delivery systems are unlikely to change. Even more threatening is the possibility that they will begin to offer these services themselves. The future of your organization depends on seizing these opportunities.
At Elder Services of the Merrimack Valley (ESMV), an Area Agency on Aging (AAA) serving older adults and people with disabilities who reside in Northeast Massachusetts, we have embraced the promise embodied in the changing health care partnership landscape. We recognized that with traditional government-based sources of funding stagnating or diminishing, we had to be creative and seek out new revenue areas that could help us branch out and achieve sustainability. It became apparent that there were opportunities through health care partnerships to expand our capacity, bolster our financial position and advance our core mission.
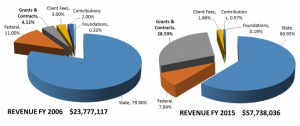
And while ESMV’s journey to health care collaboration has not always been easy, our efforts have paid off in terms of extended consumer reach and diversification of our funding. From 2006 to 2015, we’ve been able to grow the share of ESMV revenue that comes from grants and contracts by almost 25 percent, from about 4 percent 10 years ago, to around 25 percent today.
Where and how will the changes that need to take place happen?
I like to tell staff at ESMV that we already have many of the tools the health care players need. Health care partners seek to evolve into a stronger, higher quality and affordable health care system. If the growing emphasis will be on giving consumers better tools and information to navigate their care, to find the services and benefits they need to remain living longer and more independently in the community, then the aging and disability networks must be part of the solution. While we have to meet the health care partners half way across this bridge, our changes will be more about measuring our outcomes and remaining responsive to the dynamics that influence health care delivery. While we need to learn to work with a larger integrated team and learn their language regarding performance and risk, we should take comfort that these partnerships are consistent with our mission and purpose. We need to recognize that there will be various health care partners and this means that we have to be responsive and flexible to their needs as well as our consumers…but this can be a win-win.
This leads us to the “fit.”
Is our mission to provide care management, community services etc.? Or is it to help empower consumers while improving the quality of the services they depend on to live a full and independent life? Providing the services and programs we offer within the context of a health care partnership should always serve the larger mission of our organization. Luckily, these services are fully consistent with each other and not at odds. Sometimes this integrated care work takes us into the direction of serving a broader population, in regards to either age or income. However, the focus will be based on the need for our services. This is the guiding principle of our collaboration with health care, and we’ve seen that what we do is in high demand.
I would encourage leaders to consistently demonstrate the passion they have for seizing these new opportunities and to share their vision and confidence in their staff and Board members to embrace the culture changes that will surely come.
Finally, I would also strongly advocate that leaders never stop educating themselves about these issues. This is a complex topic, and staying on top of it will require new learning. Luckily, the Aging and Disability Business Institute is THE place to go for CBOs looking to build or strengthen their capacity to partner with health care.
There are lots of helpful resources on “Culture Change,” including a webinar from January 2016 on the topic, in which I and my colleague from the disability community, June Sauvageau, go into detail about the steps needed to begin this process. Check it out at the link below. And remember that, while daunting, positioning your organization for the care delivery system of the future is a win-win for you and your clients. Go out there and start making it happen.
Rosanne DiStefano has been Executive Director of Elder Services of the Merrimack Valley, Inc. (ESMV) since 1985. ESMV is an organization known for its innovation and leadership both in aging policy and community-based programs. ESMV has also been at the forefront of creating stronger delivery systems for dually eligible elders and adults, creating bridges and creative partnerships with a number of health care entities, including Senior Care Organizations, Accountable Care Organizations, and Medical Homes.
Additional Resources:
Leadership and Change Management for Community-Based Organizations
Strategies to Strengthen Organizational Culture to Drive Performance